Free Women's Health Physical Therapy
Informational Event!
Mary Nalls PT, MPT and her Pelvic Health Team from Physical Therapy Your Way PLLC would like to invite you to our FREE informational event on Wednesday, November 20th at 7 p.m. Please watch the video below and call to register today!
Please Watch Our Video
Register Now for our
FREE Informational Event.
Or call:
571-312-6966
The first 20 to register receive a free 15 minute screen
Learn about...
-
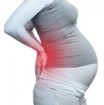
Pregnancy Related Pain
-
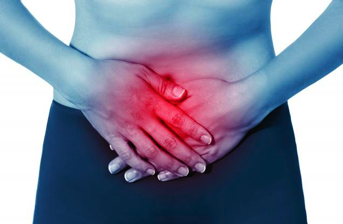
Pelvic Pain & Painful Sex
-
Incontinence (Leakage)

-
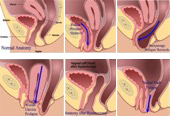
Pelvic Organ Prolapse
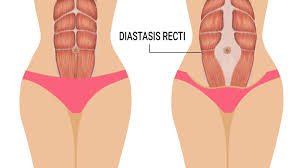
Abdominal Muscle Separation
Spaces are limited! Register online
or call 571-312-6966 Today!

